
Voice of domestic helpers: things are better in Hong Kong, but we don’t want to stay
28 February 2017
In the shadow of Hong Kong’s prosperity, mental illness and despair
28 February 2017New study: Zika may be linked to another brain disease
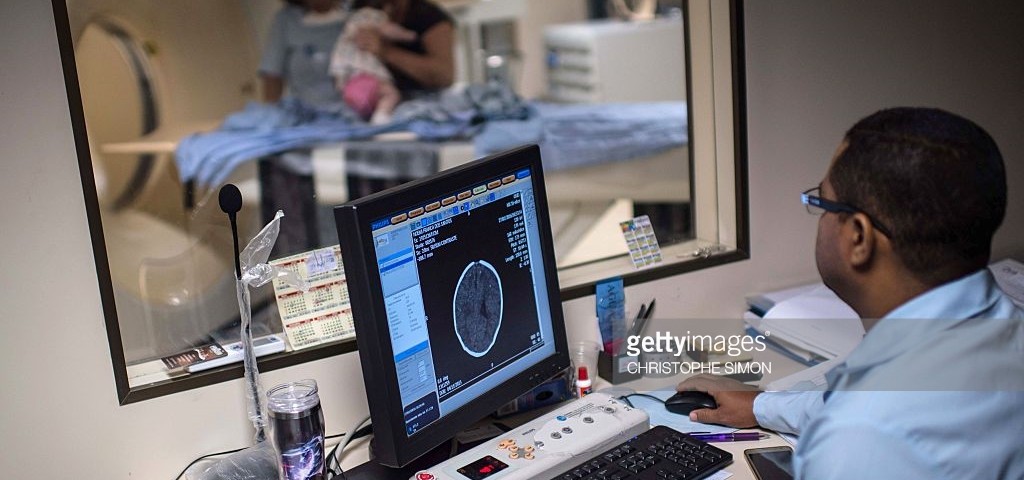
By Kevin Lui
The World Health Organisation says there is now “scientific consensus that Zika virus is a cause of microcephaly and Guillain-Barré syndrome (GBS)“, but a new small-scale study finds that the virus may also be linked to another autoimmune disorder similar to multiple sclerosis (MS).
Researchers at the Restoration Hospital in the Brazilian city of Recife followed people with symptoms of being infected by the same family of virus as Zika, who sought care between December 2014 and June 2015. All of them came with fever followed by a rash, while some also had severe itching, red eyes, as well as muscle and joint pain.
Among them, 151 cases developed neurological symptoms between December 2014 and December 2015. Six had symptoms consistent with autoimmune disorders affecting the nervous system.
After more tests and blood tests, two of the six were diagnosed with acute disseminated encephalomyelitis (ADEM), and brain scans showed that their brains’ white matter was damaged. The four others were diagnosed with GBS, whose association with Zika has increasingly been agreed upon by the scientific community.
All six of them were found to have been infected with the Zika virus.
ADEM attacks the myelin, the coating around nerve fibres, causing the brain and spinal cord to swell. Unlike MS, it usually consists of one single attack that most sufferers will recover from within six months; yet in some cases, the disease can reoccur.
“This doesn’t mean that all people infected with Zika will experience these brain problems. Of those who have nervous system problems, most do not have brain symptoms,” Maria Lucia Brito Ferreira, one of the study’s authors, tells the American Academy of Neurology.
“However, our study may shed light on possible lingering effects the virus may be associated with in the brain,” adds Ferreira.
Five of the six diagnosed with autoimmune disorders still had problems with motor functioning when they were discharged from the hospital. In addition, one of them had vision problems, and another’s memory and thinking skills were affected.
“These findings from Brazil suggest that clinicians should be vigilant for the possible occurrence of ADEM and other immune-mediated illnesses of the central nervous system,” James Sejvar from the US Centers for Disease Control says.
He also hopes that ongoing probes into Zika and immune-related neurologic diseases will provide answers as to why the virus “appear[s] to have this strong association with… immune/inflammatory diseases of the nervous system.”
The findings will be presented later this month at the American Academy of Neurology‘s 68th Annual Meeting in Vancouver, Canada.
“Though our study is small, it may provide evidence that in this case the virus has different effects on the brain than those identified in current studies,” says Ferreira.
– See more at: http://jmsc.hku.hk/reportinghealth2016/2016/04/12/study-zika-another-brain-disease/
